 Significant bleeding usually occurs from at least three different sites. In addition to signs and symptoms of the underlying condition, those of DIC are associated with bleeding and/or inappropriate clotting. Signs and symptoms of DIC depend upon the underlying condition, such as infection, trauma or malignancy, and on the severity and the extent of DIC. Cancer is one of the most common causes of low-grade DIC. With chronic DIC, the predominant feature is typically increased clotting, not bleeding. Simultaneous clotting and bleeding can occur with chronic DIC, but in most cases this is a lower grade, persistent clotting activation process and the body has sufficient capacity to compensate. This chronic form of DIC is difficult to recognise and is much less often diagnosed. Most cases of DIC that are diagnosed develop rapidly and suddenly ( acute), but there are cases in which it develops gradually, occurring over a longer period of time. Other less common causes, such as snake bite venom, toxic drug reaction, blood transfusion reaction, organ transplant, or frostbite.Organ failure, such as liver or pancreas.Cancers, such as acute promyelocytic leukemia or tumours that develop within glands (adenocarcinoma) cancer cells may release a pro-coagulant.Pregnancy and childbirth, for example when a woman has an abruption (bleeding under the placenta), or a foetus that has died (stillbirth) or amniotic fluid escapes to the lungs.Major surgery, such as cardiopulmonary bypass surgery.Trauma, such as due to an accident, head injury or significant burns.Infections, especially with severe or systemic infections (and sometimes resulting sepsis), primarily bacterial but also sometimes seen with fungal, viral, or parasitic infections.DIC can develop very quickly, becoming serious or even life-threatening in a short time. Simultaneous clotting and bleeding can occur. This can overwhelm the system to the point that the body begins to bleed excessively because platelets and clotting factors have been depleted. 
Widespread clotting can use up platelets and coagulation factors at a rapid rate. The result is the formation of a multitude of tiny clots that can block small blood vessels and prevent blood and oxygen from getting to tissues and organs, leading to multi-organ failure. With conditions that trigger DIC, the response is exaggerated, clotting is activated throughout the body, and control mechanisms are inhibited. Based on the extent of the injury, the body responds by stimulating sufficient clotting to stop the bleeding and confining it locally, that is, only at the site of injury. The body detects a pro-coagulant, a substance such as tissue factor that is released from cells when they are damaged. Normally, the body initiates haemostasis and forms a blood clot only when needed, i.e., when there is an injury and bleeding. Feedback mechanisms accelerate the clotting process, then slow it down, and control the volume of clot produced. This clotting process is tightly regulated. The clot stays in place until the injury is healed, then other factors break the clot down (fibrinolysis) and remove it. Then coagulation factors are sequentially activated (see coagulation cascade) to produce a net of fibrin threads that weave through the platelet plug and form a stable clot. First, platelets adhere to the injury site and clump together, forming a loose plug. Typically, when a person has an injury to a blood vessel and bleeding occurs, the body stops the bleeding by initiating a process called haemostasis. This abnormal activation of blood clotting mechanisms can develop as the result of a variety of diseases and conditions. Because the clotting uses up coagulation proteins and platelets, excessive bleeding can occur. 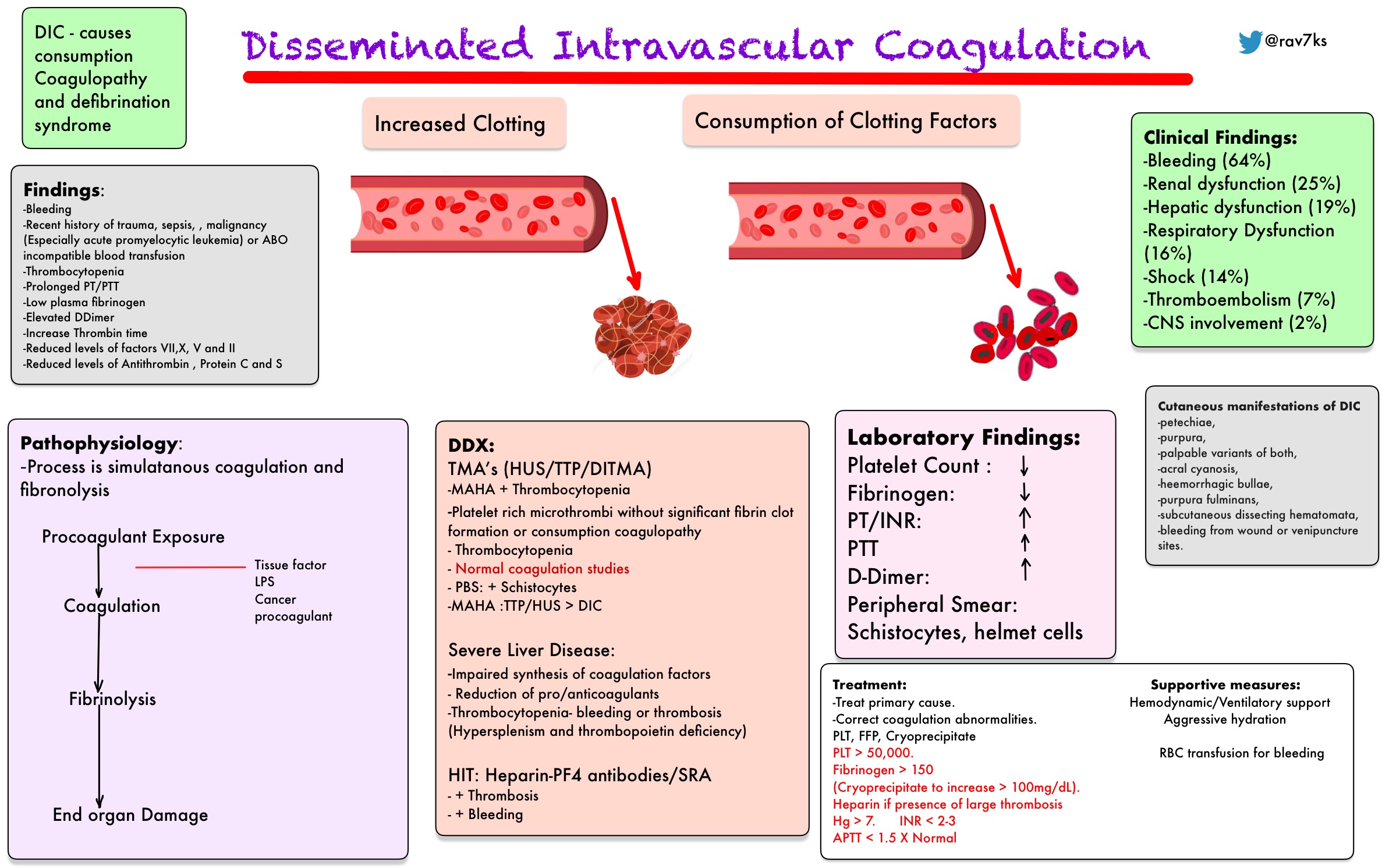
This can disrupt normal blood flow to organs such as the kidneys and liver and can lead to organ failure. Blood clots form in small blood vessels throughout the body. Urine Protein and Urine Protein to Creatinine Ratioĭisseminated intravascular coagulation (DIC) is a serious, sometimes life-threatening condition in which the proteins in the blood involved in blood clotting become overactive.Urine Albumin to Creatinine Ratio or ACR.Unvalidated or misleading laboratory tests.Red Blood Cell (RBC) Antibody Identification.Heparin-induced Thrombocytopenia Antibody.Genetic Tests for Targeted Cancer Therapy. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
